For further reading on clinical presentation, diagnosis and management I would refer you to these two articles. 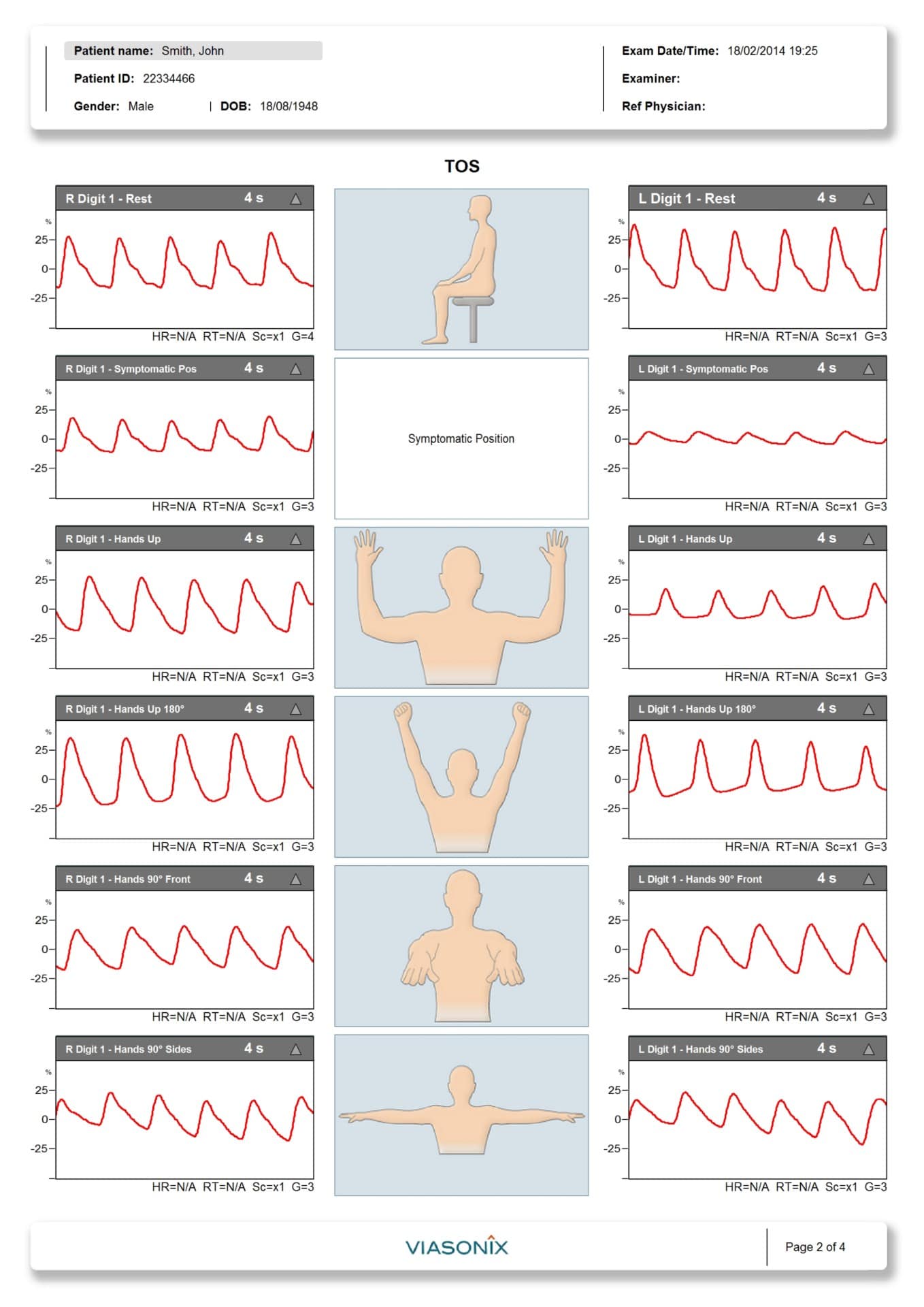
It was one of the best sources I came across in this body of research and applicable to every day clinical practice. Watson and colleagues provide a two-part masterclass which comprehensively outlines the musculoskeletal examination required to arrive at the diagnosis of TOS, and provide treatment strategies to manage scapular dyskinesia, muscular imbalances and improve container dysfunction. 
“Diagnosis of symptomatic thoracic outlet syndrome is dependent on a systematic, comprehensive upper-body examination” (Watson et al, 2009, p.588). The diagnosis of thoracic outlet syndrome remains disputed as there is no standard objective test to confirm clinical impressions. It remains a diagnosis of exclusion (Hooper, et al., 2010, p. So what exactly can we look for in our clinical assessment to assist with diagnosis? DIAGNOSIS & CLINICAL PRESENTATION Often it is difficult to say specifically where the point of compression is and radiological and electrophysical testing can present as normal. It is also know that presentation of these symptoms vary from patient to patient. It is known that TOS is a cluster of neurological, pain and vascular deficits that sit on a continuum from intermittent to permanent impairments. Thoracic outlet syndrome remains a diagnosis of exclusion and recent studies have revealed that it can take up to 60 months (5 years) for patients with symptomatic TOS to gain an appropriate diagnosis. Symptomatic TOS comprises over 80% of all people presenting with this diagnosis. That is to say there is a huge proportion of patients will present with no radiological or electrophysical abnormality (Hooper et al., 2010a Sanders et al., 2007 Kaczynski et al., 2013). The second category is Neurological TOS, which is broken down further into true and symptomatic TOS. The first category is Vascular TOS, which includes arterial and venous and accounts for ~ 5% of all presentations. In the current research trials, thoracic outlet syndrome is being classified into the following categories: CLASSIFICATION OF THORACIC OUTLET SYNDROME Thoracic outlet syndrome was first described in 1927 by Adson and colleagues and known at this time as scalenus anticus syndrome. The formal term that most authors refers to as Thoracic outlet syndrome was derived by Peet and colleagues in 1956. Thoracic outlet syndrome (TOS) is a syndrome/condition that encompasses a cluster of upper extremity symptoms which are due to compression of the neurovascular bundle by various structures in the area just above the first rib and behind the clavicle. The three most common regions where compressions is thought to occur is the intrascalene triangle, the costoclavicular triangle and the subcoracoid space. Seven years later and I am excited to share a revised piece that includes the latest ideas around clinical assessment, and in particular sensory testing in the differential diagnosis of this challenging condition. Recently I listed to a fantastic podcast by Jo Gibson through Clinical Edge on Thoracic Outlet Syndrome and was thrilled to learn some advances which have taken place in our knowledge of this condition since I first published a blog on the topic in 2013.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
